If A&E departments currently find themselves in a ‘complete state of crisis’ then it is likely that there are two main challenges creating this situation. They are:
Excessive demand for services
Blockages that are caused when patients cannot easily be released for onward support
There are digital solutions that can help with both challenges, but the remedy requires a wider transformation of care systems. This is because the ability of an A&E unit to achieve the seismic change needed to tackle these problems is, by itself, limited. Digital solutions will not work in isolation.
Having spent some time working with A&E departments recently, we have seen first hand the challenges caused by demand and the subsequent need for a multifaceted response.
There is a popular narrative that many patients don’t need to be in A&E, and that is probably true. But the patients don’t know whether they actually require A&E services or not. They may even have been directed there by 111, the experts that the public relies on.
Helping patients understand what to do when they need assistance is clearly important. Equally, once patients are assessed as needing a clinical intervention, they should be referred to the most appropriate option from the many that are available. As mentioned earlier, misdirected patients only contribute to the demands on the system and cause blockages in patient flow. If A&E services have the right data, which follows the patients who are subsequently directed to the correct service point, then the flow of patients through the care system will be improved.
This is a system-wide challenge that needs system-wide thinking
Many hospitals face issues at both the front and back doors. This is a care system-wide issue. We are almost embarrassed to say that, it is so obvious. Patients who are medically fit for discharge but occupying beds, for various reasons, mean that new patients cannot flow through the care system in the right way and the flow becomes blocked.
Ambulance services in the UK lost over a million hours last year because vehicles that could have been responding to patients were stuck outside emergency departments (EDs) waiting to hand patients over. Sending out more ambulances to respond to calls just leads to bigger queues on their return, so the only answer in the long term is to take fewer people to the hospital in the first place.
This doesn’t mean refusing to respond to those in need. Instead, we must recognise that many people that call for an ambulance could have better alternative options. Of the nearly 22,000 incidents received by ambulance services via 999 each day in December 2022 (source NHS AQIs), over 80% require dispatch of a 5-tonne double-crewed ambulance. Over 50% are conveyed to ED when in reality a large percentage end up being discharged with no further intervention or could be directed elsewhere to care in the community or pharmacies if the system knew more about them.
The system needs to start working together to do everything it can to keep you out of the hospital and, where it is safe, identify when an ambulance is not needed. Ultimately this will lead to a faster response time for genuine emergencies.
The accident and emergency demand funnel
At a system level, it is possible to see demand as a funnel. The aim is to ensure that digital interventions maximise high-quality clinical time with fewer patients.
Managing patient experience upstream of A&E is key to managing demand. Patients are actually a key part of the care workforce, ideally using self-care and preventative approaches to health to make sure they remain as well as possible, solving less serious problems as and when they have them.
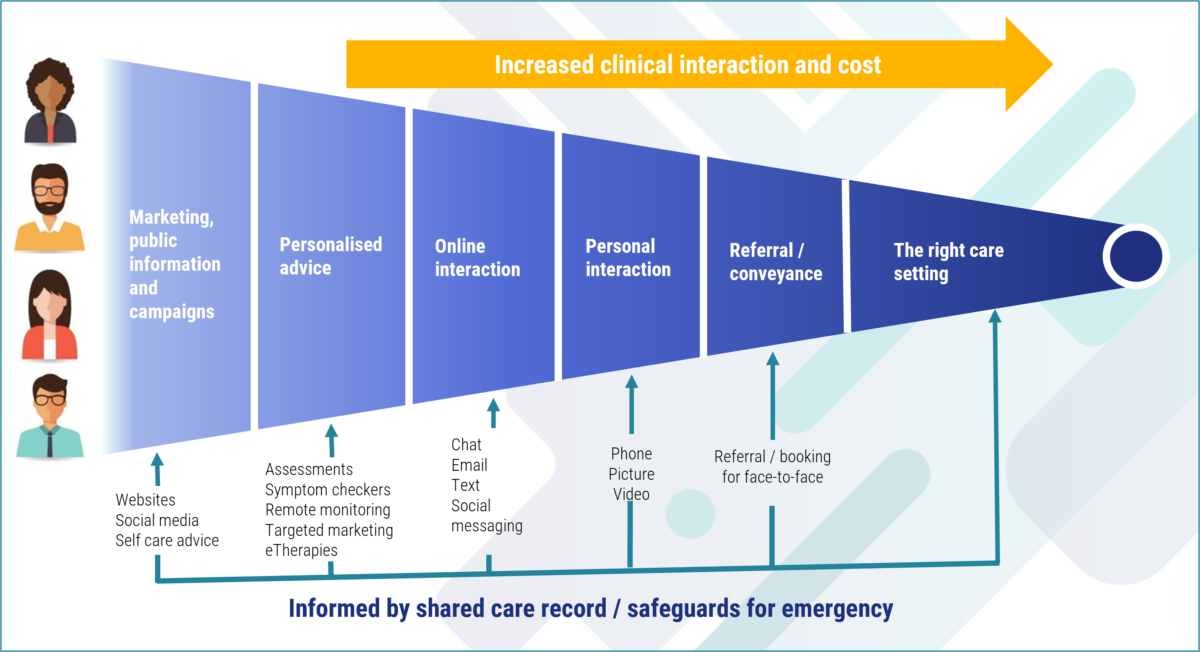
Technology has a big part to play in empowering patients and the wider public to contribute more to their care and achieve good clinical outcomes. The aim is to empower people to help themselves in the following ways:
– Understand their condition.
– Take advantage of new technology like wearables that can monitor conditions and online content to guide actions.
– Manage initial interactions with care services online, with an increased level of personalisation provided by tooling such as online triage and supporting booking.
– Redirect themselves to the most appropriate service points.
The more effectively we can support these activities, the more we can reduce demand and pressure on A&E.
The opportunity for digital strategy to support urgent and emergency care
Trusts are exploring these solutions; however, we have not seen a concerted strategy to align the range of tools in the market to the challenges faced by A&Es in a clear way. What we need is a strategy and plan where the value and benefits are articulated and the risks and issues mitigated.
The diagram below shows eight families of technology solutions that can be used to support four common A&E patient segments to achieve two key goals: reducing attendance and improving flow.
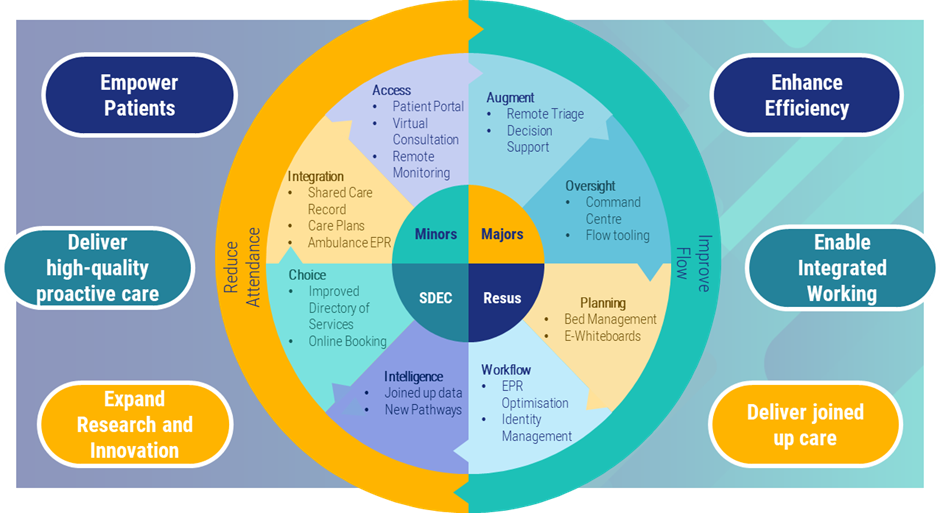
Although there’s much more nuance in how A&Es operate, this model is broadly right. For minor injuries (Minors) and same-day emergency care (SDEC), the focus is on reducing admission after an A&E attendance. For major injuries (Majors) and patients requiring resuscitation (Resus), the focus is on designing mechanisms for improving flow when admission is required.
Applying this line of thinking there are eight families of solutions, which need to be used together to make a holistic digital solution. There is no single vendor that has a platform which enables this to happen. Still, there are lots of elements which could be brought together under an umbrella digital strategy for unscheduled care.
Once you have a strategy, then you can be confident that there is capability, capacity and utility in the vendor market to help you deliver it.
Creating an emergency care strategy
A digital strategy for unscheduled care is like any other digital strategy. The issue of integrating technology and data to enable clinicians to operate at the top of their licenses is common. However, the pressure is now. Hopefully, some of the thinking in this short blog will provide confidence in the potential of digital to comprise an important part of the solution.
We’d love to talk about how we could support you in this next stage of planning. Please contact us to see how we can help.
About the authors

Andy Haywood
Andy joined Channel 3 from the Welsh Ambulance Services NHS Trust (WAST), where he was CIO and a member of the board. Before WAST, hey worked in large acute trusts and NHS Digital, delivering complex programmes, cyber-security and policy roles. Prior to his NHS career, he was an officer in the Royal Navy for 12 years.
